How Can I Determine If I Qualify For Medicaid
Qualifying for Medicaid is not as black and white as qualifying for most other government programs. Most government programs have some basic requirements along with very clear income guidelines to help individuals know if they qualify.But Medicaid has many ways that someone can qualifyand even though income makes up part of the eligibility requirements, it is not solely based on that. Even people with the lowest incomes may not qualify for Medicaid if they do not fall into one of the Medicaid groups.
And people who make a middle-range income may qualify if they fit one of the qualifying groups and can fall back on options such as share of cost
If you are pregnant and uninsured, Contact your local Medicaid office to find out if Medicaid is the right option for you.
Compiled using information from the following sources:
1. US Government Information
What Is The Cost
None. Medicaid law prohibits states from charging deductibles, copayments, or similar charges for services related to pregnancy or conditions that might complicate pregnancy, regardless of the Medicaid enrollment category. HHS presumes pregnancy related services includes all services otherwise covered under the state plan, unless the state has justified classification of a specific service as not pregnancy-related in its state plan. States may, however, impose monthly premiums on pregnant women with incomes above 150% of FPL and charge for non-preferred drugs.
Most states that cover pregnant women in their CHIP program do not have cost-sharing or any other fees associated with participation in the program.
How Can I Get Financial Assistance While Pregnant
Read Also: Vagisil Safe For Pregnancy
Texas Has A Program For Pregnant Noncitizens But The Program Doesn’t Actually Care For Them
There is one category of patients who pose a particular conundrum for obstetric providers in Texas: immigrants. The state has the highest number of births to noncitizens outside of California, and many of those women are low-income. The large majority can’t access pregnancy Medicaid, even though most other states allow longtime legal residents to participate.
Texas does have a prenatal care program for noncitizens. There’s a huge caveat, however: It doesn’t actually cover the mother, just the fetus she is carrying. It may be the ultimate example of the state’s fragmented maternal care system and how that system prioritizes babies.
The program dates back to President George W. Bush, who extended the Children’s Health Insurance Program to cover unborn babies. At the time, the idea the fetus is a child and a future citizen and should therefore receive prenatal care attracted more attention for its anti-abortion origins than for its potential to help immigrant mothers. In many of the 16 states that have adopted it, the type of care women receive isn’t much different than what they would get under pregnancy Medicaid.
For example, CHIP Perinate only covers labor if the result is an actual delivery . Premature or “false” labor when the mother goes to the hospital with contractions that turn out to be nothing isn’t covered. Nor does CHIP pay for a mother’s nonobstetric emergencies, like a rotten tooth in danger of turning septic or hospitalization for a serious illness.
Will A Marketplace Health Plan Also Cover A Newborn
Yes. The ACAs EHB requirement mandates coverage of maternity and newborn care. Newborn care covers childbirth and immediate care for the baby after birth. The specifics of this coverage will vary by state and by each individual plan, but all women in Marketplace coverage must also enroll their baby in coverage soon after birth.
If the newborn is eligible for Marketplace coverage, then the parents can choose to add the baby to the familys existing Marketplace plan or choose a new Marketplace plan for the baby. If they opt for the latter, they can enroll the baby into a new Marketplace plan at any metal tier. However, when enrolling a newborn into Marketplace coverage, other members of the household are generally not permitted to change their existing Marketplace coverage.
Also Check: Getting Braces While Pregnant
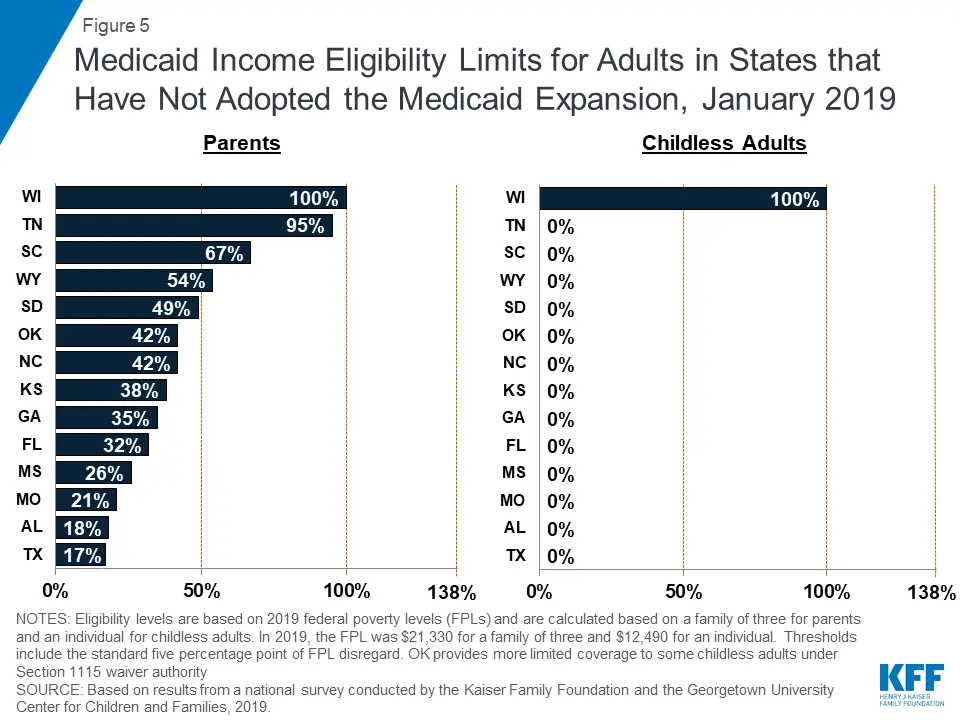
Pregnancy Medicaid Income Limits
Medicaid often denies pregnant women because their household income exceeds the limit established by their state. Therefore, you do not want to over-report your earnings or live in a region with a low threshold.
Uninsured women who make too much to qualify for Medicaid still have many options, including CHIP, private insurance, moving to another state, and the medically needy program.
Reduced Coverage / Medicare Cost Sharing Or Premium Payment
Qualified Medicare BeneficiariesCovered group: individuals covered by MedicareIncome limits: Income cannot exceed 100% of the federal poverty level. For more information, view the Guidelines for Medicare Cost-Sharing Programs brochure.Age: Medicare beneficiaries of any ageQualifications: Individuals must be eligible for Medicare Part A hospital insurance.
Specified Low-Income Medicare BeneficiariesCovered group: individuals covered by MedicareIncome limits: Income cannot exceed 135% of the federal poverty level. For more information, view the Guidelines for Medicare Cost-Sharing Programs brochure.Age: Medicare beneficiaries of any ageQualifications: Individuals must have Medicare Part A
Qualified IndividualsCovered group: individuals covered by MedicareIncome limits: Income cannot exceed 135% of the federal poverty level. For more information, view the Guidelines for Medicare Cost-Sharing Programs brochure.Age: Medicare beneficiaries of any ageQualifications: Individuals must have Medicare Part A
You May Like: Can Donating Plasma Hurt An Unborn Baby
How Can I Apply For Lamoms
You must fill out an application form. If needed, someone can assist you in completing the form. You can get an application form from the Medicaid office in the parish where you live, at any of the participating Medicaid Application Centers, from our Web site by clicking here, or by calling 1.888.342.6207. The application form with your information can be mailed to your local Medicaid office.
Early And Periodic Screening Diagnostic And Treatment
The Early and Periodic Screening, Diagnostic and Treatment benefit provides comprehensive and preventive health care services. EPSDT is key to ensuring that children and youth receive appropriate preventive, dental, mental health, developmental and specialty services.
All Health First Colorado coverable, medically necessary services must be provided even if the service is not available under the state plan to other people who qualify for Health First Colorado. Benefits not listed are not considered to be a state plan benefit and are therefore outside of EPSDT coverage and exceptions. No arbitrary limitations on services are allowed, e.g., one pair of eyeglasses or 10 physical therapy visits per year.
Who Qualifies?
Children and Youth ages 20 and younger who are enrolled in Health First Colorado.
Top Benefits:
- Providing physical, mental, developmental, dental, hearing, vision, and other screening tests to detect potential problems
- Arrange for corrective treatment as determined by child health screenings
- Lead Screening
Co-pay Costs:
Children under the age of 19 do not have co-pays. Co-pay costs for youth ages 19 and 20 vary, see program information page.
| Program Information Page |
Also Check: Is It Safe To Donate Plasma While Breastfeeding
If You May Qualify For Medicaid Or Childrens Health Insurance Program
- Medicaid and CHIP provide free or low-cost health coverage to millions of Americans, including some low-income people, families and children, and pregnant women.
- Eligibility for these programs depends on your household size, income, and citizenship or immigration status. Specific rules and benefits vary by state.
- You can apply for Medicaid or CHIP any time during the year, not just during the annual Open Enrollment Period.
- You can apply 2 ways: Directly through your state agency, or by filling out a Marketplace application and selecting that you want help paying for coverage.
- Learn how to apply for Medicaid and CHIP.
Is A Woman Who Has Access To A Family Members Employer
Possibly. If the employer-sponsored insurance is unaffordable or not MEC, the woman is eligible for APTCs. Affordability is determined by the IRS standards for the percentage of income a person is expected to spend on insurance. This calculation applies to the cost of the employees insurance, not the cost of the family plan. That means that if the premiums for the employees insurance are affordable, no member of the family is eligible for an APTC. If the individuals premium is unaffordable, the family will be eligible for APTCs in an amount determined by their income and the premium cost.
Also Check: Donate Plasma While Pregnant
What Changes When A Woman Already Enrolled In Medicaid Becomes Pregnant
Generally, nothing. A woman who was previously eligible and enrolled in full-scope Medicaid who becomes pregnant continues to be eligible, and will be able to access pregnancy services. A woman who becomes pregnant while enrolled in Medicaid Expansion can stay in that coverage, at least until redetermination. The state must inform the woman of the benefits afforded to pregnant women under other coverage categories, such as pregnancy-related Medicaid, and provide the option to switch categories if the woman is eligible.
Monitoring Substitution Of Coverage In Chip

States are required to include in their state plan a description of procedures used to ensure that CHIP coverage does not substitute for coverage under group health plans. States use various procedures to prevent substitution of coverage, such as monitoring survey data or private insurance databases, or applying a waiting period for individuals who are no longer enrolled in private coverage. This requirement can be found at section 2102 of the Social Security Act. Additional information on states specific CHIP waiting period policies.
Read Also: Can I Drink Breakfast Essentials While Pregnant
Can I Choose My Own Doctor Through The Lamoms Program
You may use any doctor who is enrolled as a Medicaid provider.To get a list of doctors, dentists or other medical service providers in your parish who take Medicaid, please visit our Provider Map page. This page will let you search for Medicaid services in your parish. If there is no doctor listed in your parish, try searching for doctors in your region or in the parishes around yours.
You can also call 1.877.455.9955 toll-free for a listing of specialists in your area who are enrolled and active in Medicaid programs.It is important to remember that not all doctors who are active in the Medicaid program are taking new patients. Be sure to ask the doctors office if they are taking new Medicaid patients when you call to schedule an appointment. If you have private insurance in addition to LaMOMS, be sure to ask if your doctor accepts Medicaid as a “secondary” payer.
Traveling To Another State
If you’re traveling to another state and fall ill, you may be out of luck Medicaid won’t cover the cost of services in a state that isn’t your home state. Generally, you can only use your Medicaid coverage out-of-state if you encounter a true life-threatening emergency that requires immediate care .
That said, sometimes, pre-approved treatment at an out-of-state facility is covered by Medicaid, but only when proper authorization is obtained. Similarly, Medicaid coverage may kick in if you receive treatment in an out-of-state facility that borders yours, and in which residents of your state routinely seek care. Again, you must make sure Medicaid will cover such care before pursuing it, or you risk getting stuck with the associated bills.
Maurie Backman has been writing professionally for well over a decade, and her coverage area runs the gamut from healthcare to personal finance to career advice. Much of her writing these days revolves around retirement and its various components and challenges, including healthcare, Medicare, Social Security, and money management.
Recommended Reading: Early Pregnancy Implantation Rash
Can An Uninsured Woman Enroll In Marketplace Coverage Upon Giving Birth
Maybe. If the baby is eligible for Marketplace coverage, then the baby qualifies for an SEP as a new dependent. In such instances, the regulations will also permit an SEP for the new mother, as someone who has gained a dependent through birth.
WOMEN ALREADY ENROLLED IN FULL-SCOPE OR EXPANSION MEDICAID
Do Marketplace Health Plans Provide Women With Comprehensive Coverage Including Maternity Care
Yes. All Marketplace plans must include the ten Essential Health Benefits , one of which is maternity and newborn care. HHS has not specified what must be covered under this category, delegating that authority to the states. Thus, specific benefits covered under maternity care vary by state.
2. What changes when a woman enrolled in a Marketplace plan becomes pregnant?
Nothing, unless she wants it to. The woman may choose to remain in a Marketplace plan or, if eligible, to enroll in Medicaid or CHIP. The woman will not lose eligibility for the APTCs as a result of access to MEC through full-scope or pregnancy-related Medicaid, but cannot be enrolled in both simultaneously and thus must choose. In deciding which coverage to select, overall cost, access to preferred providers, impact of transitioning across plans, and effect on family coverage influence preference.
Read Also: Can You Donate Plasma When Pregnant
Action Steps For States
- States must add counseling and pharmacotherapy benefits for pregnant women, which under Section 4107 of the Affordable Care Act are now mandatory benefits under Medicaid. This coverage is defined as diagnostic, therapy, counseling services, and pharmacotherapy for cessation of tobacco use by pregnant women. For more information, please see State Medicaid Director Letter #11-007 and contact your regional CMS office.
- Promote cessation benefits to pregnant women and all women of reproductive age.
- Make use of the many resources available to the public and to health care providers to help women quit smoking. See this Resource Guide for a list of highlighted resources.
For technical assistance and additional resources, contact .
Your Local Health Department Can Help You Find Affordable Prenatal Care
Your local health department can connect you to the services that can keep you in prenatal care while youre pregnant.
If youre at a low income and eligible, Presumptive Eligibility for Pregnant Women will be your first step toward prenatal coverage. PEPW is temporary coverage that can keep you healthy early in your pregnancy before Medicaid kicks in.
In Florida, the Department of Children and Families determines Medicaid eligibility for prenatal care. After PEPW, Medicaid will cover you for the rest of your pregnancy.
Healthy Start offers services to pregnant women, infants and children up to age three. Services include: provider referral, ongoing care coordination, and childbirth, breastfeeding and parenting support.
You May Like: Using Vagisil During Pregnancy
Do I Qualify For Medicaid
Medicaid provides free or low-cost health coverage to some low-income people, families and children, pregnant women, the elderly, and people with disabilities. Many states have expanded their Medicaid programs to cover all people below certain income levels. Medicaid qualifications depend partly on whether your state has expanded its program.
How Long Can I Get Services From Moms & Babies
You may be able to get coverage for services beginning up to three months before you apply. You can get services throughout your pregnancy and for 60 days after you have your baby. If you have Moms & Babies when your baby is born, your baby can get All Kids for one year.
All Kids Hotline 1-866-ALL-KIDS
TTY: 1-877-204-1012
Read Also: Accidentally Donated Plasma While Pregnant
Can I Apply For Medicaid If Im Not Pregnant
You can’t take it with you: If you’re relocating, you’ll need to reapply for Medicaid in the state where you’re planning to reside.
Q. Can I use my Medicaid coverage in any state?
A: No. Because each state has its own Medicaid eligibility requirements, you can’t just transfer coverage from one state to another, nor can you use your coverage when you’re temporarily visiting another state, unless you need emergency health care.
Medicaid offers health coverage to millions of Americans, and in many states, that coverage matches or even surpasses that of private health insurance. Medicaid is jointly funded by the federal government and state governments, but each state has the option to set its own rules and requirements for eligibility. As such, transferring your Medicaid coverage from one state to another isn’t always possible.
Programs For Pregnant Women
Snapshots are informational only. You must apply to find out what programs or waivers you qualify for.
If you are not looking to find coverage for pregnant women, please choose another category.
Also Check: Is It Okay To Use Vagisil While Pregnant
Get Important News & Updates
Sign up for email and/or text notices of Medicaid and other FSSA news, reminders, and other important information. When registering your email, check the category on the drop-down list to receive notices of Medicaid updates check other areas of interest on the drop-down list to receive notices for other types of FSSA updates.
What If Im Turned Down By Medicaid
- You may be able to buy a private health plan through the Marketplace instead for the 2018 plan year in the fall. You may qualify for savings based on your income through a premium tax credit and savings on out-of-pocket costs.
- If you don’t qualify for either Marketplace or Medicaid savings, you still have options. Learn more here.
Recommended Reading: Sore Breasts After Mirena Removal

