What To Expect During A C
For any pregnant woman preparing to give birth, there are times when the baby is breech or the mother experiences unexpected health issues. In these cases, an emergency C-section may take place to keep the mother and baby as safe as possible.
While the C-section can potentially be a last minute surprise addition to the birth plan, a woman with type 1 diabetes may need to plan and be prepared for a C-section in advance. There are a number of reasons that you may include a C-section in your birth plan, such as the size of your baby, retinopathy or kidney issues. An early delivery may also be scheduled if you have had a previous C-section, or due to maternal or fetal health issues.
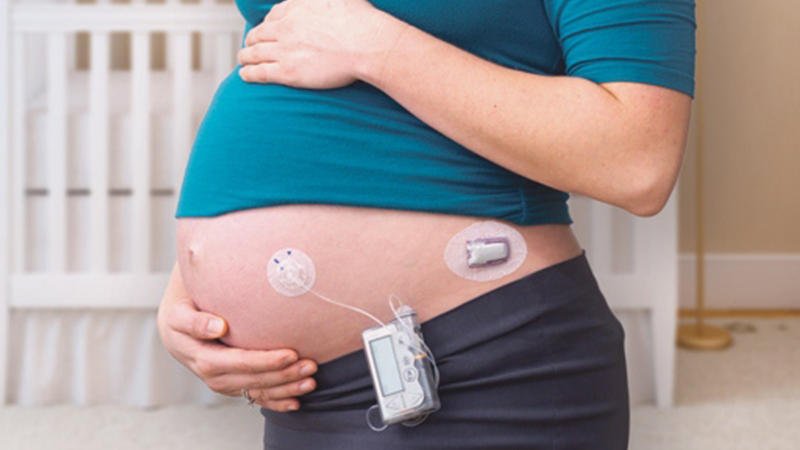
If your C-section is scheduled, you will have the opportunity to discuss the plan well before the actual birth. Some medical teams are comfortable letting the patient and their caregiver manage type 1 diabetes during the birth, while others prefer to assign a doctor to this task throughout the surgery. If you wear an insulin pump, continuous glucose monitor , or other type 1 diabetes device, you may need to remove it prior to the surgery, but again, this is at the discretion of you and your medical team.
The C-section surgery itself takes about an hour, though everyones surgical experiences vary.
What To Consider Prior To Pregnancy
Pregnancy is both a physical and an emotional journeyits no wonder women with type 1 diabetes who are pregnant have many questions and concerns. That is why preconception planning is absolutely crucial. Having said that, some pregnancies are unplanned. It is important to speak with your doctor and diabetes care team and get the guidance that you need to have a healthy pregnancy with T1D as soon as you know you are pregnant.
How soon should you start preconception planning? Working on the following goals for a few months in advance of conception can make the whole process easier and less stressful:
Glycemic Control In Labour And Delivery
Planning insulin management during labour and delivery is an important part of care and must be adaptable given the unpredictable combination of work of labour, dietary restrictions and need for an operative delivery. The goal is to avoid maternal hypoglycemia while preventing significant hyperglycemia which, in turn, may increase the risk of neonatal hypoglycemia . Options for peripartum BG control include watchful waiting until BG rises above a specified threshold , presumptive initiation of intravenous insulin infusions or continuing with CSII therapy. In a retrospective study of 161 consecutive women with type 1 diabetes, women who chose to continue on CSII during labour had better glycemic control than women using CSII during pregnancy but who chose to convert to intravenous insulin infusion during labour. There was no increase in maternal hypoglycemia, suggesting that the continuation of CSII during labour and delivery appears safe and efficacious . Similarly, another retrospective study found that women using CSII had excellent glycemic control without hypoglycemia . Observational studies comparing the use of CGM to SMBG during labour and delivery identified improved glycemic control with CGM however, neonatal hypoglycemia was comparable between groups . Each centre should establish protocols which include BG targets, monitoring frequency, insulin regimen and intravenous glucose, based on nursing, medical and anaesthesia expertise available, and patient choice .
Read Also: Can I Drink Breakfast Essentials While Pregnant
Preparing For Pregnancy With Type 1 Or 2 Diabetes
The first thing to do is talk to your GP or diabetes team. They may refer you to a specialist pre-conception care team.
You should get information about how diabetes affects pregnancy and how pregnancy affects diabetes. You will also be given details of local support you can have during pregnancy, including emergency contact numbers.
Having diabetes should not affect your fertility . Talk to your doctor if you have any concerns about your fertility.
There are several steps you can take before getting pregnant that will give you the best possible chance of having a healthy pregnancy.
How Does Diabetes Affect Female Fertility
Diabetes of both kinds can cause infertility issues in women. However, the woman can get pregnant after proper glycemic control.
Staying pregnant is a different matter altogether. Diabetes can make it difficult for women to stay pregnant, especially if they have had the disease for long. Diabetes causes a lack of glucose control in the body, and this could make the implantation of the fertile egg in the uterus difficult. Also, diabetic women may be obese this contributes to problems too. Fertility doctors have even said that women who have diabetes usually get pregnant every month when they are fertile, but there is no point since the egg is usually unable to implant within the uterus this results in a miscarriage even before the pregnancy has started or the woman realizes she is pregnant. The chances of miscarriage in diabetic women increase by anywhere between 30 to 60%. There are other risks too, even if implantation has occurred there is a higher risk of birth defects, the baby might be larger and an increased risk of gestational diabetes can prove harmful to the mother and the child.
Recommended Reading: Vagisil Cream While Pregnant
Fact: Women Who Prefer Multiple Daily Injections Can Have Very Healthy Pregnancies Too
An insulin pump and continuous glucose monitor are two tools that can certainly help many women achieve better blood sugar management before and during pregnancy but it can be done with multiple daily injections , too.
The trade-off of using MDI to manage your diabetes instead of an insulin pump is that youll need to take many more injections per day. If you arent willing to take an additional injection to bring a 160 mg/dL blood sugar down to 100 mg/dL, for example, then using MDI during pregnancy may not be the right choice for you. Pressing the buttons on a pump to receive those extra doses of insulin might be easier for you.
Another challenging aspect that comes with MDI is that none of todays long-acting insulins have been studied for their safety in pregnancy. There is no reason to believe any of these insulins are harmful to a baby, either, but there just isnt any data on it. Women have been using these insulins during pregnancy over the last decades with the outcome of healthy, beautiful babies!
If possible, every woman with type 1 diabetes should consider using a CGM before/during/after pregnancy to make healthy blood sugar levels more achievable. Trying to achieve this range without a CGM can mean pricking your finger to test blood sugar at least 10 to 15 times per day. A CGM will give you so much more information, support, and safety compared to constant finger pricks.
Pcos And Type 2 Diabetes
PCOS stands for polycystic ovarian syndrome, a condition in which hormonal imbalances create multiple cysts on a woman’s ovaries, leading to unpredictable menstrual cycles and infertility. Research has shown a strong correlation between PCOS and Type 2 diabetes .
In addition to erratic menstrual cycles, PCOS can also cause women to miss their periods altogether, or produce immature eggs. Both PCOS and Type 2 diabetes are characterized by unhealthy levels of blood glucose and a resistance to insulin. A variety of medications can be prescribed to help lessen or reverse the effects of PCOS. Metformin is one of the most popular drugs. Metformin was prescribed for diabetes long before it was found to be successful in the treatment of polycystic ovarian syndrome . As with Type 2 diabetes, a healthy lifestyle can also go a long way toward reducing or eliminating PCOS . The key is to bring blood sugar levels into a normal and stable range while combating insulin resistance.
In some instances, women who are neither unhealthy nor overweight develop Type 2 diabetes and polycystic ovarian syndrome. Hispanic and African-American women also have a greater likelihood of being diagnosed with PCOS .
Diabetes doesn’t preclude men and women from reproducing. It does, however, require professional guidance, meticulous maintenance of health, and monitoring of blood sugar and hormonal levels. With proper care and attention, the vast majority of diabetics can have healthy offspring.
Read Also: Is Kinesio Tape Safe For Pregnancy
Target Blood Glucose Levels During Pregnancy
Recommended daily target blood glucose numbers for most pregnant women with diabetes are
- Before meals, at bedtime, and overnight: 90 or less
- 1 hour after eating: 130 to 140 or less
- 2 hours after eating: 120 or less3
Ask your doctor what targets are right for you. If you have type 1 diabetes, your targets may be higher so you dont develop low blood glucose, also called hypoglycemia.
What Is The Treatment For Gestational Diabetes Mellitus
Specific treatment for gestational diabetes will be determined by your doctor based on:
-
Your age, overall health, and medical history
-
Extent of the disease
-
Your tolerance for specific medications, procedures, or therapies
-
Expectations for the course of the disease
-
Your opinion or preference
Treatment for gestational diabetes focuses on keeping blood glucose levels in the normal range. Treatment may include:
-
Special diet
-
Insulin injections
You May Like: Is It Ok To Use Vagisil While Pregnant
Can A Teenager Get Type 1 Diabetes
Without insulin, sugar cannot travel from the blood into the cells, and high blood sugar levels can occur. People can develop type 1 diabetes at any age, from early childhood to adulthood, but the average age at diagnosis is 13 years. An estimated 85% of all type 1 diagnoses take place in people aged under 20 years.
What It Means For You
If you have type 1 or type 2 diabetes, you may be at higher risk of having:
- a large baby which increases the risk of a difficult birth, having your labour induced or needing a caesarean section
- a miscarriage
People with diabetes are at risk of developing problems with their eyes and kidneys .
Some people with type 1 diabetes can develop diabetic ketoacidosis, where harmful chemicals called ketones build up in the blood.
Pregnancy can increase your risk of developing these problems or make existing ones worse.
Don’t Miss: Using Vagisil During Pregnancy
Can Type 1 Diabetes Cause A Miscarriage
The short answer is yes, but the more complete answer is that people with well-managed T1D have no more risk for experiencing miscarriage than their peers without diabetes.
Chronically high blood sugars at the time of conception make you twice as likely to experience a spontaneous miscarriage compared to a non-diabetic pregnancy, explains Jennifer Smith, diabetes care and education specialist at Integrated Diabetes in Wynnewood, Pennsylvania, and co-author of Pregnancy with Type 1 Diabetes.
Yes, unmanaged blood sugars are a huge cause of early miscarriage, but well-managed blood sugars are not, Smith says.
This is why people with T1D are heavily encouraged to achieve an A1C at or below 7.0 percent before intentionally conceiving.
To clarify, having the occasional high blood sugar around the time of conception does not cause miscarriages.
What Smith is describing is the negative impact of long-term high blood sugar levels and persistently high A1C levels during the months leading up to and during the beginning of your pregnancy.
If youre going to miscarry due to unmanaged diabetes, it will likely happen very early, in the first 8 weeks of pregnancy, she says.
Its important to remember, though, that for most women with reasonably healthy blood sugar levels, its 99 percent likely that your diabetes was not the cause of your miscarriage, Smith adds.
The health of your uterus is just as affected by those long-term high blood sugar levels.
Type 2 Diabetes: Blood Sugar And Fertility

Perfect timing is required to become pregnant. That’s why, generally speaking, couples aren’t advised to consult an infertility specialist unless they’ve been trying to conceive for one year without success . It’s simply that tough to get the timing right. Unfortunately, Type 2 diabetes can complicate ovulation and make a woman’s menstrual cycles highly unpredictable. That makes it all the more difficult to become pregnant.
In most cases, Type 2 diabetes is caused by being overweight, obese and/or in poor physical shape for an extended period of time . The extra weight leads to insulin resistance. When one hormone is out of balance it can cause other hormones to become imbalanced, as well. Since insulin is a hormone, a domino effect can be triggered affecting testosterone, estrogen, progesterone and other hormone levels that are key components of reproduction. Such imbalances are associated with everything from erectile dysfunction to cysts on ovaries .
Infertility specialists encourage their patients with Type 2 diabetes to focus their efforts on eating healthy, exercising, losing weight and closely monitoring blood sugar levels . Taking vitamin supplements is also encouraged. If those efforts alone don’t lead to a healthy pregnancy, then medications like metformin, clomiphene citrate and letrozole may be introduced to improve fertility.
Read Also: Can I Donate Plasma While Breastfeeding
How Can I Manage My Diabetes During Pregnancy
The Pregnancy in Diabetes Program manages patients with gestational diabetes and pre-gestational type 1 and type 2 diabetes. The goal of the Program is to provide comprehensive care to meet the full range of women’s needs before, during, and after pregnancy. In addition to care during pregnancy, preconception consultation is available with specialists in maternal-fetal medicine and endocrinology to better ensure that women enter pregnancy with type 1 or type 2 diabetes well-informed and as healthy as possible.
What is diabetes? What is insulin? How does diabetes affect the body? Marie McDonnell, M.D., Chief of the Diabetes Section of the Division of Endocrinology, Diabetes, and Hypertension at Brigham and Women’s Hospital, answers patients’ most commonly searched questions about diabetes.
Significance Of Decreasing Insulin Requirements
In contrast, results from other studies found no association with decreasing insulin requirements and birthweight, and neonatal weight distribution . However, 1 study observed a trend for greater LGA neonates in women with decreasing insulin requirements . Caution is required when interpreting the findings as researchers used differing calculation methods to indicate fall in insulin requirements or perhaps due to heterogeneity in the population of women with type 2 diabetes included in the studies. The use of advanced sonographic and fetal doppler assessment in the surveillance of the fetus at risk, as in other high-risk pregnancies, may allow further stratification of risk in this population, but the optimal indicator of feto-placental compromise, particularly in women with diabetes, remains unclear.
In summary, the impact of decreasing insulin requirements is still not certain. While fetal monitoring in this situation can provide reassurance of current fetal well-being, it should not be viewed as a substitute for a well thought out plan for timing of delivery that takes into consideration other risks for perinatal mortality, such as gestational age, maternal glycemic control , prepregnancy retinopathy , maternal age, obesity and smoking history.
You May Like: Is It Bad To Donate Plasma While Pregnant
How Diabetes May Affect Your Baby
Babies born to women with diabetes are often much bigger, a condition called “macrosomia.”
Because their mothers have high blood sugar levels, they get too much sugar through the placenta. The baby’s pancreas senses it and makes more insulin to use it up. That extra sugar gets converted to fat, making a large baby.
Many hospitals keep an eye on babies of mothers with diabetes for several hours after birth. If you regularly have high blood sugar levels while you’re pregnant , your baby may get dangerously low blood sugar right after they’re born. Their insulin is based on your high sugar, and when it’s suddenly taken away, their blood sugar level drops quickly and they’ll need glucose to balance it out.
Their calcium and magnesium levels may be off, too. Those can be fixed with medication.
Some babies are too big to be delivered vaginally, and you’ll need a cesarean delivery, or c-section. Your doctor will keep an eye on your baby’s size so you can plan for the safest way to give birth.
Management: Healthy Behaviour Interventions
Weight gain. The 2009 IOM guidelines for weight gain during pregnancy were developed for a healthy population and little is known regarding optimal weight gain in women with GDM. Retrospective cohort studies of GDM pregnancies show that only 31.7% to 42% had GWG within IOM guidelines. Those gaining more than the IOM recommendations had an increased risk of preeclampsia , caesarean deliveries , macrosomia , LGA and GDM requiring pharmacological agents . Modification of IOM criteria, including more restrictive targets of weight gain, did not improve perinatal outcomes of interest . A large population-based study including women with GDM, concluded that while pre-pregnancy BMI, GDM and excessive GWG are all associated with LGA, preventing excessive GWG has the greatest potential of reducing LGA risk . These researchers suggest that, in contrast to obesity and GDM prevention, preventing excessive GWG may be a more viable option as women are closely followed in pregnancy.
Further studies are needed to develop weight gain guidelines for GDM patients and to determine whether weight gain less than the IOM guidelines or weight loss in pregnancy is safe. Until this data are available, women with GDM should be encouraged to gain weight as per the IOM guidelines for the BMI category to reduce adverse maternal and neonatal outcomes and postpartum weight retention.
You May Like: Is It Safe To Donate Plasma While Pregnant
Who Will I Work With To Manage My Diabetes During Pregnancy
In the Pregnancy in Diabetes program, our specialists in maternal-fetal medicine, endocrinology, and nutrition, work together to ensure that women with type 1, type 2 and gestational diabetes achieve healthy pregnancies. Our specialists are also available to provide both preconception consultation and postpartum management.
Emphasis is placed on achieving blood sugar control during pregnancy through a combination of lifestyle changes such as diet, exercise and medication, if needed. The team works closely with primary care providers to facilitate a successful transition to long-term care, ensuring focus on each patients individual needs. The Diabetes in Pregnancy Program provides easy access for women requiring appointments with multiple specialists. Learn more about our Pregnancy in Diabetes Program.

