Report Adverse Drug Reactions In Pregnancy
Report any suspected adverse drug reactions in the mother or child following use of a medicine in pregnancy, including adverse pregnancy outcomes such as congenital malformations or adverse neurodevelopment outcomes, on a Yellow Card.
When reporting ADRs related to medicines used in pregnancy, the following information is particularly valuable for our assessment of the report:
-
Timings of when the medicine was taken during the pregnancy
-
The outcome of the pregnancy
-
Details of any relevant family history, including any obstetric history
-
For reports concerning congenital malformations, a detailed clinical description of any congenital anomaly and the results of any imaging , or laboratory tests
-
For reports concerning adverse developmental outcomes, whether the child has met their key developmental milestones and whether they have had any further health issues
Please include any other relevant information including other medications or substances taken during the pregnancy, as well as folic acid intake.
Report Yellow Cards electronically using:
Seizure Frequency During Pregnancy
Because the appropriate gold standard comparator group has not been employed, the American Academy of Neurology concluded that there is insufficient evidence to determine if seizure frequency changes occur in WWE during pregnancy . There has been wide variation in the reported range of women experiencing increased seizure frequency during pregnancy . This variance may be due to differences in study populations and in other methodological issues. In addition, given the known pharmacokinetic changes during pregnancy, assessment of blood levels is needed in future studies . To provide more informed therapeutic strategies to maintain seizure control during pregnancy, clarification of factors that contribute to individual variance in increased seizures is important. Based on a number of studies from the literature, there is suggested increased seizure risk during pregnancy for lamotrigine and oxcarbazepine, both of which are glucuronidated for elimination . One positive finding concluded by the AAN found that WWE who were seizure free in the 912 months prior to pregnancy had an 85% chance of remaining so during pregnancy .
Planning For Pregnancy When You Have Epilepsy
At one time, women with epilepsy were advised never to get pregnant. Thats not the case anymore.
For most patients, having epilepsy should not prevent you from having children. However, there are challenges to consider and plan for with your doctor.
The potential effect of seizures and medications to control them create unique concerns during pregnancy. Approximately 24,000 babies are born to women with epilepsy every year the overwhelming majority of which are healthy.
Research published in August 2022 found that women with epilepsy may be at increased risk of depression and anxiety symptoms during or after pregnancy compared with peers. Today, there are pregnancy-safe treatment options for both conditions.
While some planning is important, it is possible to have a healthy pregnancy while managing the challenges associated with epilepsy.
You May Like: How Long Does It Take To Get Pregnant After Iud
Is It Safe To Take Anti
It is really important that you DO NOT STOP or decrease the dose of your antiepileptic medication during pregnancy without a doctors direction as this can be unsafe for both you and your unborn baby.Most women , taking anti-epilepsy medication will have a normal pregnancy and deliver a healthy baby. Anti-epilepsy medication taken during pregnancy can affect some babies, but it may not harm your baby as much as having seizures during the pregnancy.In any pregnancy there is a risk that a child may have a malformation , learning problems or autism. This risk is higher if you are taking anti-epileptic medication. How much the risk is increased depends on many factors, such as the type of medicine, the dose of medicine, the number of anti-seizure medicines you are taking. The risk seems to be highest for women:
- taking sodium valproate
- taking more than one anti-seizure medication
- taking high doses of anti-epilepsy medications.
If you find out that you are pregnant you should urgently make an appointment to see your doctor. Your doctor will assess whether it is safe to change your medication or decrease the dose. Read more about the risks and benefits of taking anti-epilepsy medicines.
Sodium Valproate An Important Case

Sodium valproate has greater risks in pregnancy than other ASMs, with 7 women in 100 having a baby with a major malformation, rising to 1 in 10 women if they take more than 1000mg per day.
Also, up to 4 children in 10 whose mothers took sodium valproate have problems with development and learning.
The MHRA states that sodium valproate should not be prescribed to girls or women who are pregnant, or who may become pregnant in future, unless it is the only effective drug for them and they are on a pregnancy prevention programme .
They also recommend that treatment with sodium valproate should only be started by a doctor experienced in managing epilepsy.
If you are taking sodium valproate, do not suddenly stop taking it, but talk to your doctor as soon as possible about the best treatment options for you. Sodium valproate is an effective drug for epilepsy and for some women, it is the best or only drug that controls their seizures.
You May Like: Can You Bleed When Your Pregnant
How Might My Epilepsy Affect My Baby And Me After Birth
Caring for your baby postpartum can be a concern for moms with epilepsy. To reduce the risk of an injury to your little one if you do happen to have a seizure, try changing baby’s diapers on the floor or bathing your child with other adults around .
Breastfeeding your baby shouldnt be a problem, however. Most epilepsy medications pass into the breast milk in such low doses that they are unlikely to affect a nursing baby.
Seizures Vs Medication: The Risks Of Both
Although some types of anti-seizure medication carry risks to the unborn baby, seizures also carry a risk to both mother and baby.
Dr. Krishnamurthy says that a seizure in pregnancy involves a risk of direct harm to the fetus, maternal bleeding, miscarriage, and risks to the mothers health. If you add up statistically, all of those risks, it is estimated that the risk of some type of harm occurring either to the mother or to the fetus from a single seizure may be as high as 20% per seizure, she explains.
Anti-seizure medications carry the risk of both physical malformations and cognitive or developmental challenges. Dr. Krishnamurthy says the risk of malformations with older-generation drugs is about 610% while the risk with newer medications is about 4%.
Cognitive and developmental outcomes are being studied in the MONEAD study, which so far suggests that children are developing normally even when exposed to newer anti-seizure medications in pregnancy.
Women with epilepsy have a very good chance of normal pregnancy outcomes if they avoid the drugs with the highest risks, and if they work with their doctor, reassures Dr. Meador.
Don’t Miss: What Can Help You Get Pregnant Faster
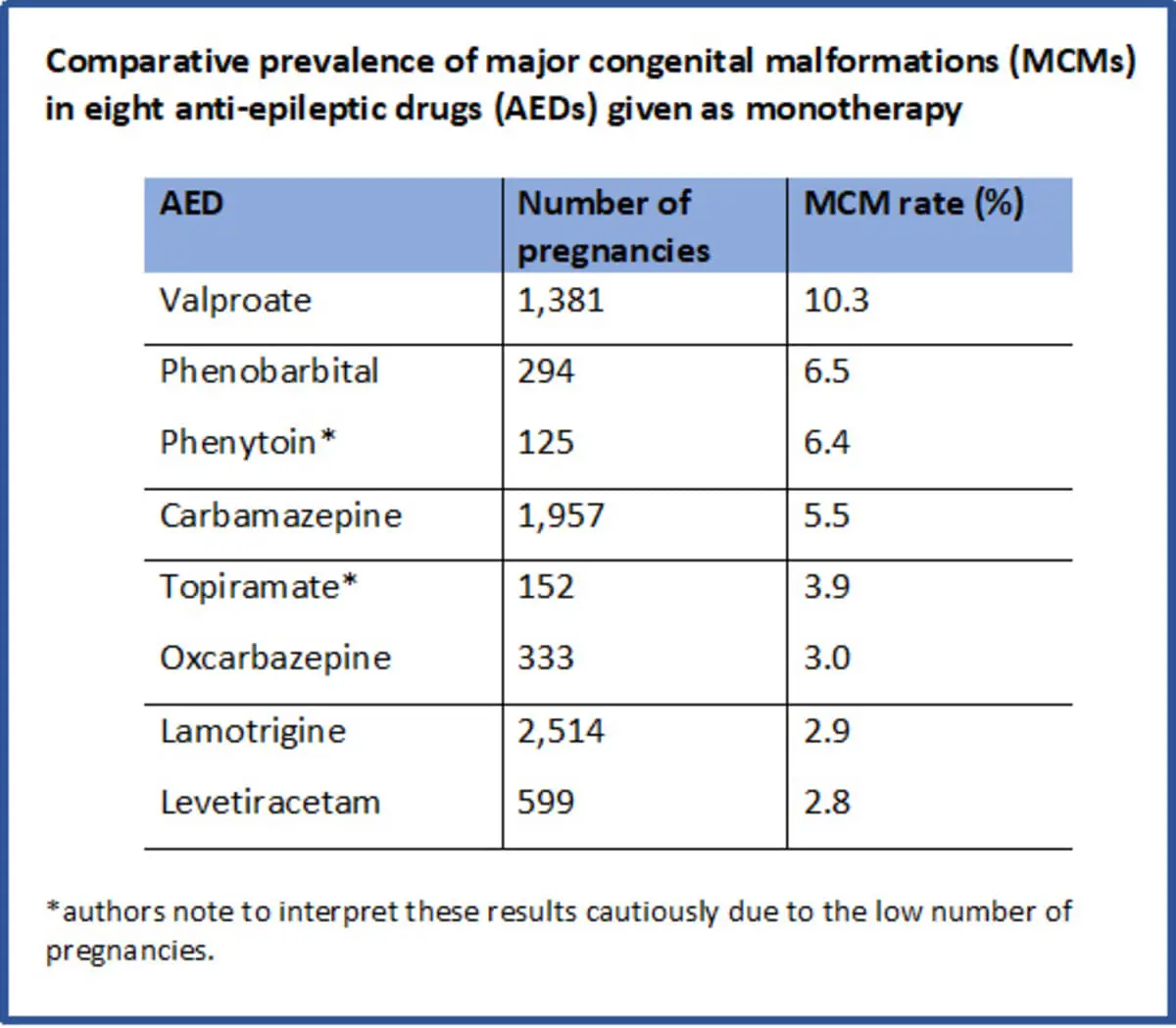
Anatomical Teratogenesis Associated With Individual Antiepileptic Drugs
Since the 1960s, AEDs have been known to have teratogenic potential. Since seizures carry the risk of potential injury or even death, most WWE cannot afford to discontinue AEDs. Therefore, it is important to delineate which AEDs produce the best seizure control while minimizing teratogenicity. AEDs taken during the first trimester of pregnancy may increase the risk of MCMs in children born to WWE. The AAN guidelines and a recent meta-analysis concluded that that risk is highest for valproate out of all the AEDs . The recent European and International Registry of Antiepileptic Drugs in Pregnancy results confirmed the increased risk for valproate, but also demonstrated dose-dependent risks for other AEDs .
Folate And Vitamin K1
All women are recommended to take folate supplements before pregnancy. It is reasonable practice to recommend routine folate supplementation, 0.5-1.0 mg/day, to all potentially reproductive women with epilepsy taking antiepileptic drugs even if they are not contemplating pregnancy. It is currently recommended that a woman with epilepsy takes folate 5 mg/day for three months before conception and for at least the duration of the first trimester. There is good evidence that folate supplementation reduces the risks of spina bifida and other malformations in large population studies, but there is no documented evidence that it further reduces teratogenic risk in women taking antiepileptic drugs.
National Health and Medical Research Council Guidelines recommend that all babies at birth are given 1 mg intramuscular vitamin K1 or a course of oral vitamin K1. Maternal oral vitamin K1, for example 10 mg/day for one month prepartum, has been recommended when enzyme-inducing antiepileptic drugs are prescribed because the drugs may potentially predispose the baby to haemorrhagic disease of the newborn. However, reports suggest that this risk is practically negligible.2
You May Like: What Foods Help Brain Development During Pregnancy
Pregnancy Outcomes With Regard To Congenital Malformations
In recent years, several AED pregnancy registries have been established leading to new insights into teratogenic risks of AEDs. Pregnancy outcomes and other issues for WWE were examined for the new AAN guidelines, which included recommendations for patient care and future research .
There is an increased risk for MCMs in children of WWE versus the general population which has a frequency of 1.62.1% at birth . There is variability in the risk estimates among studies, but a recent publication indicates 4.5% frequency for MCMs in AED monotherapy in utero exposure and 8.6% for AED polytherapy . The most common MCMs associated with AEDs are heart malformations, orofacial defects, urologic defects, skeletal abnormalities, and neural tube defects. Specific examples include but are not limited to ventricular septal defect, cleft lip/cleft palate, hypospadias, radial ray defects, phalangeal hypoplasia, and spina bifida .
Sodium Valproate And Valproic Acid
The risk of harm to your baby is particularly high with the valproate medicines sodium valproate and valproic acid.
If you’re taking a valproate medicine and are planning to get pregnant or find out that you are pregnant, do not stop taking your medicine. See a GP or neurologist immediately to discuss your increased risk and whether this is still the best treatment for you.
People living with epilepsy who are able to get pregnant must not be given a valproate medicine unless they have enrolled in a pregnancy prevention programme. This is designed to make sure they understand:
- the risks of taking valproate medicines in pregnancy
- the need to use effective contraception to prevent pregnancy
As part of a pregnancy prevention programme, you’ll need to:
- see your consultant at least once a year to discuss your treatment
- discuss the risks of your medicine and the importance of avoiding pregnancy
- sign a form stating you understand the risks to your unborn baby if you take a valproate medicine, and agree to use effective contraception throughout your treatment
Your doctor may refer you to contraception services.
Your doctor will give you an information leaflet to explain more about the risks and how to avoid them. Keep this information in case you need to refer to it again.
Recommended Reading: Are Plan B Pills In Pregnancy Test
‘i Did As I Was Told’
After the trauma of her miscarriage, Hannah knew to plan ahead the second time around. “I stopped taking sodium valproate and started taking folic acid before I became pregnant with my son, when I was 23,” she says. “I didn’t have any seizures, so I didn’t take any medication for the epilepsy, and it was a happy, healthy pregnancy. My son was absolutely fine.”
“We’d given up trying by the time I fell pregnant but I was taking daily folic acid just in case,” she explains. “When I did fall pregnant, the doctors took me off valproate because they were concerned about spina bifida and physical abnormalities to the baby.”
Due to having regular seizures, Hannah was prescribed a different anti-epilepsy drug, but it didn’t keep them under control. “Once I was into my second trimester, the doctors said I should go back on sodium valproate because the seizures could cause premature birth,” she says.
“I was told the medication only affects fetuses during the first trimester, when physical abnormalities can occur. Nobody told me about any risks to the baby as far as neurological problems,” she adds. “So I did as I was told, but even the sodium valproate didn’t stop my seizures that time.”
Hannah’s daughter was born with severe learning difficulties, has been on medication since she was 10 years old, and needs one-to-one care at school.
Summaries Of Main Evidence And Key Findings
This section summarises the main evidence considered in this review along with the key findings. The information is presented for the following antiepileptic drugs in alphabetical order in sections 3.1 to 3.10 below carbamazepine, gabapentin, lamotrigine, levetiracetam, oxcarbazepine, phenobarbital, phenytoin, pregabalin, topiramate and zonisamide. Section 3.11 summarises the data and findings on the antiepileptics less commonly used. The available clinical data on the risk of major congenital malformations, neurodevelopmental disorders and delay, and also other reproductive toxic effects were taken from the published scientific literature and included meta-analyses and epidemiological studies in pregnancy registries, national birth registers, and population-based cohorts. The key findings from the main studies are presented in tabular form in Appendices 1 to 3.For the other antiepileptic drugs that were less commonly used, the main findings are outlined in section 3.11. These medicines include brivaracetam, clobazam, clonazepam, eslicarbazepine, ethosuximide, lacosamide, perampanel, primidone, rufinamide, tiagabine and vigabatrin.
The data for diazepam, fosphenytoin, lorazepam, midazolam, thiopental sodium and stiripentol have not been reviewed given that the authorised indications for these antiepileptic drugs include status epilepticus, acute convulsions, refractory convulsive disorders or Dravets syndrome.
Don’t Miss: How Many Days To Confirm Pregnancy
Why You Shouldn’t Stop Your Anti
Even if you are taking older generation anti-seizure medications, dont stop taking your medication without consulting a healthcare provider who knows your individual circumstances. As the pregnant body changes, your medication needs can also change.
Kaarkuzhali Babu Krishnamurthy, MD, a neurologist specializing in epilepsy in pregnancy, explains that the pregnant body can break down and eliminate medication faster, leaving less available in the body to control seizures.
If however, as a seizure physician, we increase medication appropriately to keep the blood level of the medicine the same as it was before that woman was pregnant, her risk of seizures diminishes dramatically, explains Dr. Krishnamurthy.
Regular blood tests should be taken in pregnancy to ensure levels of anti-seizure medications are maintained in the pregnant body. Depending on how your body responds, you may need to decrease, increase, or change your medications entirely. But these actions should always be guided by your healthcare team.
Women should not lower their dose during pregnancy or even outside of pregnancy on their own without the doctors advice, advises Dr. Meador. Lowering the dose during pregnancy can be dangerous to both the mother and the fetus because it could result in seizures.
What Are The Risks To My Baby If I Become Pregnant
Both seizures and medications are associated with some risks. The risk of seizures is associated with seizure type. Partial seizures probably do not carry as much risk as generalized seizures. Yet, they can lead to a generalized seizure. Generalized tonic-clonic seizures are associated with increased risk to both the mother and baby. These risks include:
- Trauma from falls or burns
- Increased risk of premature labor
- Lowering of the baby’s heart rate
- Change in seizures
Seizure control is critical because the risks from seizures are greater than the risks from medications.
Don’t Miss: What Is Safe To Take For Sinus While Pregnant
Can Pregnancy Trigger A Seizure
Seizure frequency fortunately declines or remains the same in the majority of women during pregnancy. Yet in 15% to 30% of women, there may be an increase in seizure frequency, most often in the first or third trimester.
Can lamotrigine cause birth defects?
Lamotrigine does not significantly increase risk of birth defects during pregnancy, says new study. A new study has shown that babies born to women who are taking the epilepsy drug lamotrigine, do not have a significantly increased risk of birth defects such as cleft lip, cleft palate or club foot.
Will Taking Epilepsy Medicines Affect My Unborn Baby
Taking certain epilepsy medicines during pregnancy increases the risk of your baby being born with a with a physical birth defect. Some epilepsy medicines can also harm the babys growth or development. The highest risk is thought to be between weeks 1 and 13 of your pregnancy.
Some epilepsy medicines have a higher risk of harming a baby during pregnancy than others. Taking a higher dose or more than one epilepsy medicine at the same time may also increase the risk of harm. For information about the risk of individual medicines, see our list below.
Most women with epilepsy have healthy pregnancies and give birth to healthy babies. But, it is important that you get the right information and support about which medicines to take.
You May Like: Does Plan B Affect Future Pregnancy
How Should I Plan For Pregnancy If I Have Epilepsy
Before you begin trying to have a baby, request an appointment with your epileptologist and Ob/Gyn or a maternal-fetal medicine specialist. These doctors specialize in high-risk pregnancies and can provide advanced care should any complications develop.
You and your doctors will evaluate how well-controlled your seizures are and determine whether any treatment changes are needed before you become pregnant.
We urge women to take a folic acid supplement before conception to reduce the risk of neural tube defects, which affect the brain, spine, and spinal cord. Women with epilepsy may need to take more folic acid than other women up to 4 mg a day for two to three months before conception. This is because anti-epileptic drugs may decrease the amount of folic acid levels in the body. During your 20-week ultrasound, well look for malformations that AEDs can cause. This exam is effective for looking for neural tube defects.
As with any other woman trying to become pregnant, make healthy lifestyle choices:
- Avoid smoking, drugs, and alcohol
- Eat a healthy diet
- Take prenatal vitamins
Pregnant patients with epilepsy may be more likely to show symptoms of depression and anxiety than peers with or without epilepsy. Symptoms also can occur during the postpartum period.
While researchers did not find more episodes of major depression among pregnant patients with epilepsy, they did identify risk factors that include:

